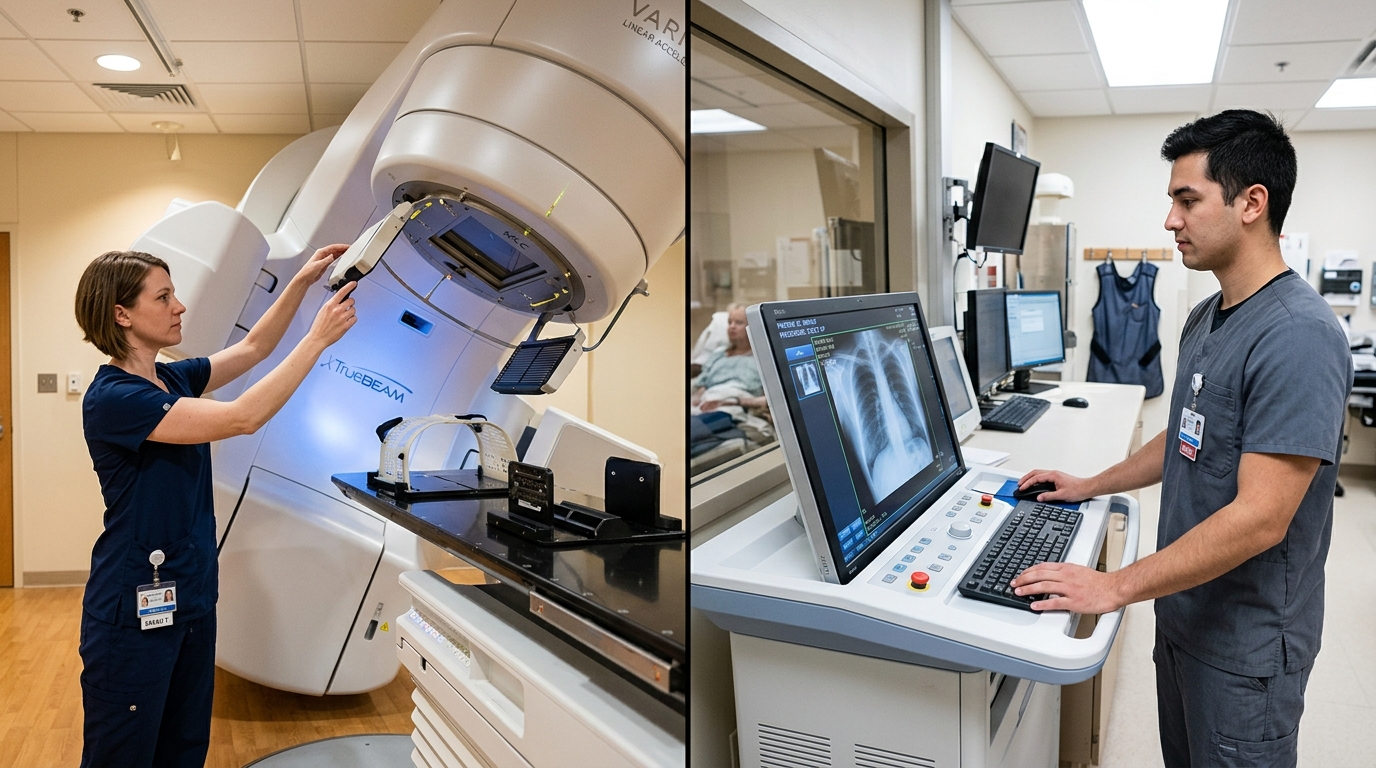
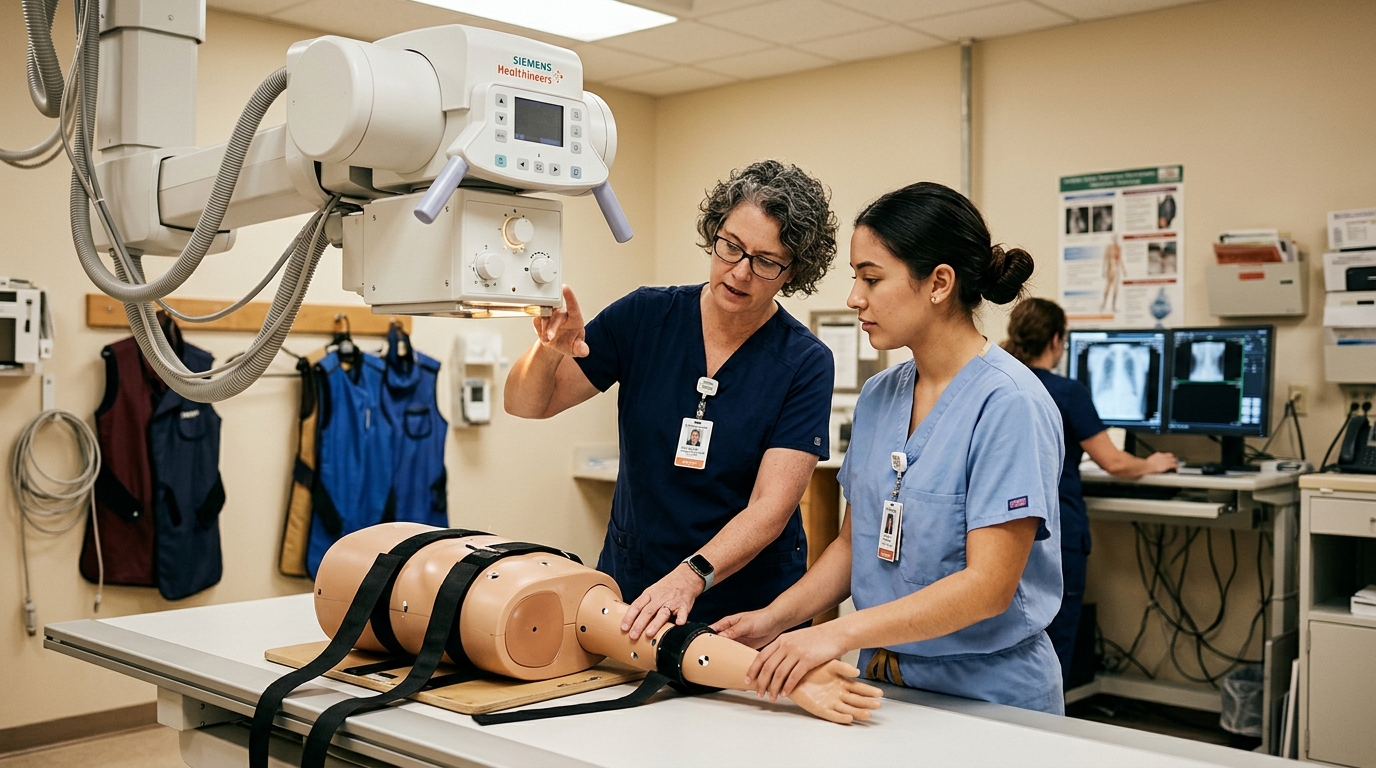
How to Ace Your Rad Tech Clinical Rotations

I remember standing in the CT control room for the first time as a student, hands shaking, completely convinced that I was going to break a million-dollar scanner just by thinking about it wrong. My preceptor, a woman named Diane who'd been doing CT for 18 years, handed me a protocol manual and said, "Read this. You're getting a hip. Be ready in ten minutes."
I'm not going to tell you it got easier after ten minutes. But I will tell you what happened: I did the best I could with what I knew, I asked questions when I was confused, and I didn't pretend to understand something I didn't. And that single interaction—that willingness to be honest about what I didn't know and to show up prepared—shaped everything that came after.
Fifteen years later, I've worked in imaging departments across four states. I've been someone who trained students, and I've been someone who trained trainers. I've seen what separates the students who get job offers before they graduate from the ones who struggle to find work. It's not brilliance. It's not always the highest test scores. It's something simpler and more important than that.
The Brutal Truth About Your Preceptor
Here's something nobody tells you directly: your preceptor isn't being paid extra to train you. They're being paid to run their department. You're an addition to their workload, at least at first.
That doesn't mean they don't care. Most preceptors care deeply about training new techs. But they're also short-staffed, stressed, and handling 12 patients today when they're usually handling eight. So your first job isn't to prove how smart you are. Your first job is to not make their day harder.
This sounds harsh, but it's actually liberating. You don't need to be perfect. You need to be prepared, self-aware, and coachable. You need to anticipate problems before they become problems. You need to be the person your preceptor can trust to not create more chaos.
I had a student once—bright kid, top of his class—who showed up to rotations every single morning without having looked at the schedule. He'd roll in, and Diane would have to tell him what department he was in that day. Meanwhile, he'd be scrambling to remember what MRI protocols look like, even though that schedule was posted the night before. Diane eventually pulled me aside and said, "I can't teach him if he's not willing to prepare. There's just not enough time."
The kid was smart. He failed his clinical rotation because he wasn't organized. That's not about intelligence. That's about whether you're serious.
The Setup: Know Your Stuff Before You Get There
Your program has given you textbooks. Use them. Not to memorize everything—that's not realistic—but to understand the fundamentals well enough that you're not starting from zero when you get to your rotation.
For CT, understand the basics of how reconstruction works, what the common protocols are (chest, abdomen, neuro, extremity), and what patient positioning looks like. You don't need to be an expert. You need to know enough that when your preceptor explains how to do a chest CT, you're filling in the gaps, not trying to understand what a CT is.
For MRI, same deal. Know the pulse sequences. Understand T1 and T2. Know what contraindications look like. This stuff is not intuitive, and nobody expects you to just absorb it in the scanner room. But if you show up having read the material, you're already ahead of 80% of students your preceptor has trained.
I always tell students: spend three hours before your first day with a YouTube video and a textbook. That three hours will save your preceptor from explaining things three times and will genuinely change how they perceive you. Not because you're suddenly an expert. Because you're clearly willing to do the work to prepare.
The First Week: Observe Like You're Being Tested
Your first week, you're probably not doing much. You're watching. And here's what matters: watch like you're studying for a final exam.
Don't stand in the corner scrolling through your phone. Be present. Ask yourself questions: Why did the tech position the patient that way? What would happen if we changed the field of view? Why did the radiologist ask for a repeat on that one image? What made it wrong?
When you see something you don't understand, write it down. Literally carry a small notebook. Write down questions, protocols you see, sequences you don't recognize, patient positioning challenges. Then, during breaks, ask about them.
I had another student—quiet, seemed kind of shy—who did this religiously. By day three, she had about 40 questions. She'd ask me in batches: "I noticed that when the patient was claustrophobic, you used a faster sequence. Is that always the case, or was it something specific about that patient?" Smart questions. Prepared questions. The kind that show you're not just standing there waiting for knowledge to osmose into you.
That student got job offers from two different hospitals before graduation. People remember the students who actually showed up mentally.
The Second Month: Start Contributing
Once you understand the rhythm a bit, you start actually doing things. And this is where a lot of students mess up because they swing too far in one direction or the other.
Some students ask permission for everything. "Can I position the patient?" "Is it okay if I take a scout?" They're hesitant to the point of uselessness. Your preceptor hired you to help, not to be a very expensive ghost.
Other students move too fast. They're confident after two weeks and taking ownership of things they actually don't understand yet. That's dangerous—not just for the patient, but because it signals to your preceptor that you're not calibrated to your own competence.
The sweet spot is somewhere in the middle. You should be actively involved, but you should be checking in. "I'm going to position this patient for a lumbar spine. Let me know if I'm missing anything." You're taking action. You're also being honest about where you are in your training.
During my travel tech years, I'd work with contractors who were fresh, and the ones who lasted were the ones who could hold both things: confidence enough to actually do the work, and humility enough to check themselves and ask for feedback.
The Relationship That Actually Matters
By month two or three, your preceptor knows whether they like working with you. And honestly? That's the only metric that actually matters.
Hospitals hire people they want to work with. You can be technically skilled but so difficult that nobody wants you on their team, and you won't get hired. You can be less experienced but reliable, pleasant, and coachable, and you'll be hired in a heartbeat. The imaging department is small, intimate, intense. You spend 12-hour shifts with these people. They're not going to hire someone they don't actually want to be around.
This doesn't mean being fake or overly agreeable. It means being genuinely professional. Show up on time. Don't complain constantly. Be willing to do the work that needs to be done without being asked four times. Use your manners. Remember people's names. Actually listen when someone's explaining something.
I'll be direct: half your clinical rotation success is technical. Half is whether your preceptor would actually recommend you to their friends. If they like working with you, they'll advocate for you. If they don't, even if you're competent, they won't.
The Question That Will Determine Your Future
Toward the end of your rotation, there's a conversation that matters more than any test: your preceptor will be asked by HR if they'd recommend hiring you. What they say in that conversation will shape whether you get a job offer.
I've seen preceptors write glowing evaluations for students who are good but not great, because those students showed up, worked hard, and were pleasant. I've seen preceptors write lukewarm evaluations for technically skilled students who were difficult, unreliable, or unwilling to listen.
The way to ensure they recommend you: be someone they would actually want to work with. Ask questions that show you're thinking critically, not just going through the motions. Thank them when they take time to teach you something. Acknowledge that you're learning and ask for feedback. Follow through on things they ask you to work on.
By the end of your rotation, if your preceptor has ever said, "I'd hire you," you're golden. That's the real credential. That's what actually opens doors in this industry.
The Practical Stuff (Because It Matters Too)
Let's talk about the boring mechanics that somehow nobody discusses:
First, your technical competency matters. You need to actually learn how to position patients correctly, how to handle equipment properly, and how to follow protocols. This is baseline. If you can't do the actual job, nothing else matters.
Second, reliability matters. Show up on time. Every single day. If you're going to be sick, call as early as possible. Don't schedule vacation during your rotation unless there's an actual emergency. Every absence makes your preceptor's day harder, and they'll remember that.
Third, communication matters. If you messed something up, say so. Don't hide mistakes. If you don't understand a protocol, ask. If you're struggling with a particular skill, tell your preceptor and ask for extra practice. Honesty is way less risky than trying to fake competence.
The Long View
I've been in this field long enough to see students from my early rotation days now working in supervisory roles, managing departments, training other techs. The ones who succeeded weren't always the smartest in the classroom. They were the ones who treated their clinical rotations like they were already professionals. The ones who showed up mentally prepared, emotionally present, and willing to work.
Your clinical rotation is only a few months of your career. But it's also the place where someone's going to vouch for you professionally. That vouch is worth way more than your GPA.
So go in prepared. Stay engaged. Be honest about what you don't know. Be reliable. Ask good questions. And remember that your preceptor is giving you a gift by spending time on your education. Respect that, and you'll be fine.